EMCsoft’s Claims Management Ecosystem assures that healthcare providers and billing companies deliver clean claims to insurance payers for proper claim adjudication. It is the integration of our versatile claims processing software Claim Agent and comprehensive fitting process called the Four Step Methodology into your claim adjudication process. This approach enables, supports, and automates your work process to maximize claim reimbursement. Request our free online demo for a great introduction into the functionality/features of Claim Agent and how it fits into your claim adjudication process.
The Software
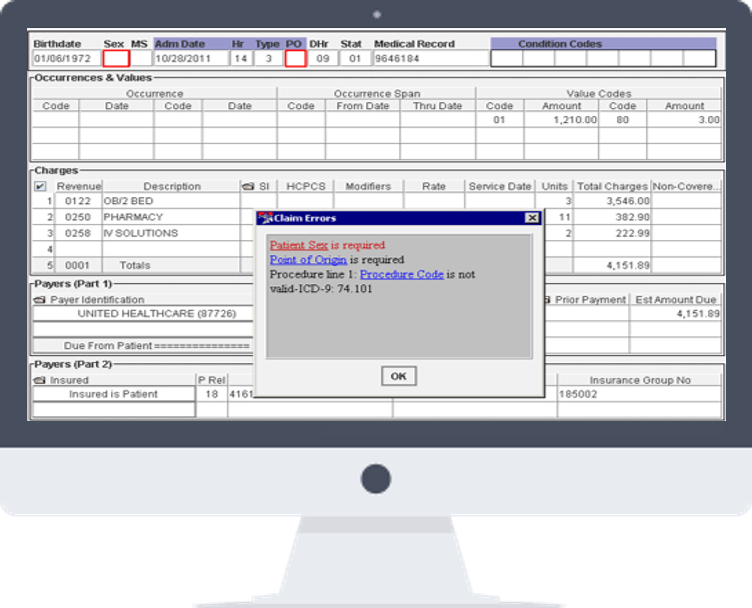
Your Claims Management Software
Claim Agent scrubs and processes your claims from the provider system to the insurance payers in a efficient, cost effective, and timely manner. The software is compatible with any system making implementation process quick and simple. We provide custom edits, bridge routines, payer lists, and work flow settings that are unique to each user.
The Fitting Process
Your Needs. Your Data. Your Cash.
Our Four Step Methodology is a unique fitting process that dramatically boosts operational and financial performance. We take a full system approach that allows for complete customization for each user to your overall workflow. This allows a range of customers from family practices to behavioral health providers to multi facility hospitals to use Claim Agent to its full potential.
Why Us
We differentiate ourselves by providing advanced customization, a platform for community of users contribute new ideas/features, and added value through strategic partnerships with industry leading organizations. Our solutions improve billing accuracy, expedite the claims process, and recover lost dollars. These results are proven by our customer loyalty and satisfaction. We provide specific examples about how the Claims Management Ecosystem has benefited our clients. Please visit the Contact Us page and fill out the form or contact us by phone.
